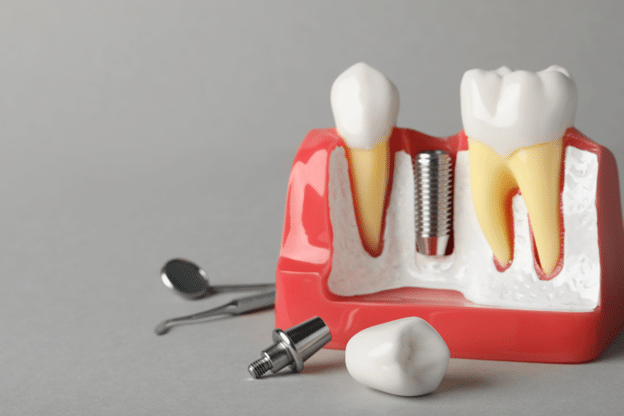
When most people start researching dental implants in Oxnard, they tend to first focus on the hardware, i.e., the titanium post and the porcelain crown. This is a natural way to begin, but it can lead to a common misunderstanding that getting a dental implant is as simple as picking a part off a shelf and installing it.
In reality, the success of implant dentistry encompasses much more than the implant itself, including the environment in which it will live.
The foundation of any successful tooth replacement is your jawbone and gum tissue. Think of this process like building a house:
You can have the highest-quality lumber and the best architectural plans, but if the soil underneath is shifting or the foundation is cracked, the structure won’t last. The state of your bone and gum health for dental implants is thus akin to the soil and foundation of a home.
Keep reading to learn how your unique anatomy influences implant planning, so you can move forward with confidence and realistic expectations for your dental implants.
Why Jawbone Density Matters
The jawbone is a use-it-or-lose-it type of tissue. When you have all your natural teeth, the roots stimulate the bone every time you chew. This stimulation signals your body to continue delivering nutrients and minerals to that specific area. Once a tooth is lost, that stimulation vanishes.
Within the first year of tooth loss, a significant amount of jawbone density can be lost because the body essentially decides that the bone is no longer needed to support a root.
For patients exploring dental implants with low jawbone density options, this biological reality is often the first hurdle to overcome because an implant requires a specific volume of healthy bone to achieve osseointegration, which is the process where the bone fuses to the titanium.
If the bone is too thin or too soft, the implant won’t have the stability it needs to withstand chewing pressure. This is why two people can walk into a clinic with the same missing tooth, but have completely different treatment paths based on how long the tooth has been missing.
Also Read: How Long Do Dental Implants Last Compared to Bridges or Dentures?
Gum Changes and Their Impact on Dental Implants
While the bone provides the strength, your gums provide the seal. Essentially, gum health is the biological gatekeeper for a dental implant. Healthy, thick gum tissue wraps tightly around the implant restoration, preventing bacteria from reaching the underlying bone. If you have a history of periodontal disease or have experienced significant recession, your implant planning will look different.
Many patients are surprised to learn about gum changes and how they affect dental implants. If the gum tissue is thin or compromised, it may not just be a cosmetic issue but a functional one. Without a robust cuff of gum tissue, the implant is more susceptible to infection.
This illustrates why maintaining a high level of periodontal health before, during, and after the process is non-negotiable for long-term success.
Why “Additional Procedures” Aren’t Just Upsells
It’s common for patients to feel a bit of sticker shock or confusion when a dentist mentions bone grafting before dental implant placement. However, these procedures are about creating a predictable outcome rather than adding unnecessary steps. Restoring bone for dental implant eligibility involves pre-treating the site to ensure it can support the load of a prosthetic tooth.
If the site isn’t quite ready, a bone graft can act as a scaffold, encouraging your body to regenerate its own bone in the area. Similarly, some patients may need a sinus lift if they are replacing upper back teeth where the bone is naturally thinner. These steps may extend the timeline by a few months, but they are the difference between an implant that lasts five years and one that lasts a lifetime.
A Case-by-Case Philosophy for Treatment Planning
One of the most important things to understand about treatment planning for dental implant procedures is that it is highly individualized. No two mouths are identical. Factors like your bite alignment, whether you grind your teeth, and your overall systemic health play massive roles.
For example, a patient with a heavy clench may require a wider implant or a different bone preparation strategy than a patient with a lighter bite.
Modern technology, such as 3D CT scans, allows us to look under the hood before any surgery begins. We can see exactly where the bone is densest and where the nerves and sinuses are located. This data-driven approach means we aren’t guessing; we are engineering a solution based on your specific anatomy.
And because we are working with living tissue, the bone and gums, we have to work at the speed of biology. Some patients may be candidates for immediate-load implants, in which a tooth is placed the same day. However, for many, the safest route involves a healing period of three to six months. This allows the bone to fully knit to the implant.
If you require bone grafting, your timeline might be longer. While it can be tempting to want the quickest fix, especially if you’re missing a front tooth, rushing the biological process is the most common cause of implant failure. Respecting the healing phases of your bone and gums ensures that, once the tooth is placed, it stays in place.
Also Read: All-on-4 vs Traditional Dental Implants: Which Option Is Right for Your Smile?
Risks of Delaying Dental Implants
If you are currently waiting to replace a missing tooth, it’s important to know that the environment in your mouth is constantly changing. Bone loss doesn’t stop; it continues over time.
The longer a gap persists, the more likely you are to need more complex procedures to restore the area. By addressing the gap sooner with an implant consultation, you often have more natural bone and gum tissue to work with, which can simplify the overall treatment.
When you’re considering dental implants in Oxnard, you want a team that prioritizes the planning phase as much as the surgical phase. You aren’t just looking for someone to place a post; you are looking for a clinician who understands how to manage your unique bone and gum architecture.
A successful result is one where the implant feels, looks, and functions just like a natural tooth, and that only happens through meticulous, biology-first planning.
Setting Realistic Expectations for Your Journey
The goal of modern implant dentistry is to restore your smile and your ability to eat the foods you love. However, the path to get there isn’t a straight line for everyone. Some patients have more ideal conditions, while others require a bit of foundational work first.
Understanding that your bone and gum conditions dictate the what, how, and when of your treatment will help you navigate the process without frustration. If your dentist recommends a graft or a specific healing period, it’s because they are looking at the long-term health of your jaw.
Expert Dental Implants in Oxnard
If you have been told you have low bone density or have concerns about your gum health, don’t let that discourage you. Options for dental implants in Oxnard with low bone density have never been better. Advances in grafting materials and surgical techniques mean that almost anyone can eventually become a candidate for implants. It’s just a matter of the right plan.
The first step is always a thorough evaluation. By looking at your bone volume and gum health today, you can get a clear, realistic picture of what’s possible for your smile tomorrow.
Ready to see what’s possible for your smile? Request an appointment at Vista Pacific Dental Care today to get started.